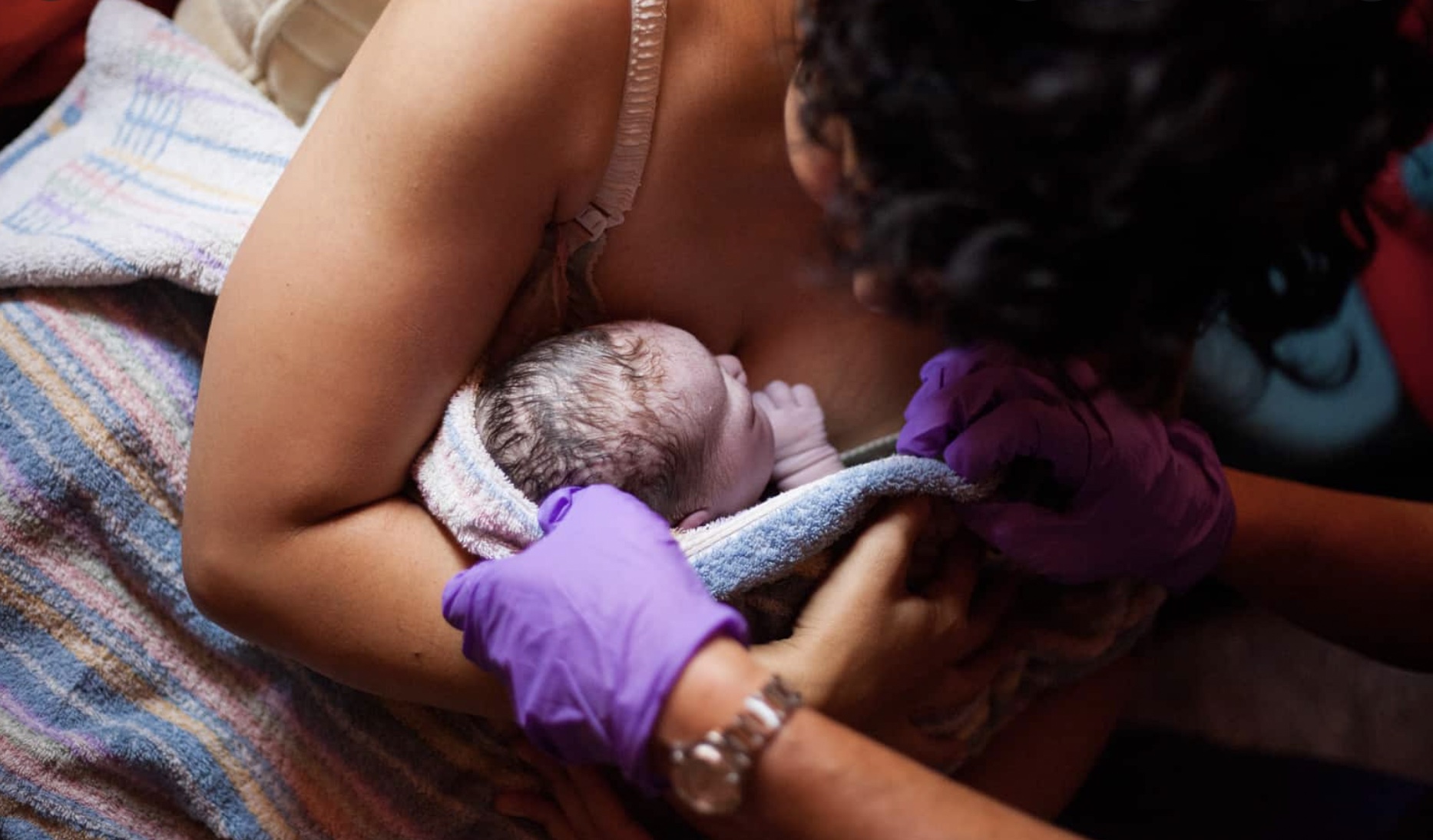
THE GOLDEN HOUR
The Golden Hour is described as “the first hour or so after birth and is a particularly awesome, miraculous, important, delicate, and intense time of transition for mother, baby, and family” (Wickman, 2020). Important elements of the Golden Hour include: delayed cord clamping, skin-to-skin contact for at least an hour, the performance of newborn assessments on the maternal abdomen, delaying non-urgent tasks (e.g., bathing the newborn) for 60 minutes, and the early initiation of breastfeeding” (Neczypor, 2017). This does not include doing any newborn procedure, such as weighing, measuring, and vitamin K injections. No poking or prodding is done during this time. The only hands that need to be on your baby are yours, and perhaps your partners. Raylene Phillips, MD, IBCLC, FAAP said this about the Golden Hour:
“This is a once-in-a-lifetime experience and should not be interrupted unless the baby or mother is unstable and requires medical resuscitation. It is a “sacred” time that should be honoured, cherished and protected whenever possible.”
MEDICALIZATION OF BIRTH
In Western Counties, birth became medicalized around the 1600’s. Before this time, birth took place at home under the care of a midwife. By the 17th century, pregnancy and birth became a point of interest by the emerging medical community and started offering hospital births to the privileged via “twilight sleep” where mama was given drugs to erase the memory of birth. As a result of this medicalization, interventions were put into practice more regularly. Childbirth became viewed less as a normal and natural experience, and more as a medical procedure. Let me be clear—I am not against interventions. In some cases, it’s the best way for your baby to be born safely into this world. But how do you know when the intervention becomes a hindrance to the natural process of birth?
Sara Wickham, midwife, speaker, bestselling author and independent researcher writes that interventions can be of great benefit, but do still come with some degree of risk (Wickman, 2020). It’s when we make interventions “standard practice” that it can become a hindrance.
As a Doula, I understand how rapidly the medical system changes. As a mother of three, I personally experienced this rapid shift in the system between my first and second births. Have you heard of the prophylaxis ointment given to newborns? During the birth of my first in 2011, it was considered standard practice to sweep neonatal prophylaxis ointment into the newborns’ eyes to minimize the risk of blindness, should the mother have gonorrhea and/or chlamydia (which I knew I did not have). But because it was “routine”, I consented to it. I didn’t know better. Then in 2012, studies proved the ineffectiveness of this practice and caregivers stopped offering it. See the Association of Ontario Midwives statement about this shift in standard practice, here. I saw firsthand how a “standard, routine practice”, something I never even questioned, could get thrown out so quickly, leaving me feeling: what else are we doing to hinder the natural process of birth and postnatal care?
So I got educated. I studied alternative, gentle and natural birthing practices. I experienced them with clients as a birth Doula and during my own three experiences. All of this knowledge led me to “6 Best Practices” that ended up being a crucial part of my birth vision list for my last birth. These 6 practices center around the first hour after baby arrives: the Golden Hour and are relevant to healthy, full-term babies.
First, I want to disclaimer this by saying that not all babies are born the same way. Those that need extra care and attention and, therefore, can’t stay with mama afterwards may need interventions like swaddling, no skin to skin, hats, etc. Remember, intervention is not all bad. It’s the misuse when it’s not needed that’s the issue. But, if you have a normal labour with no complications, then consider including these 6 practices during your third stage of labour:
1. DELAYED CORD CLAMPING
Baby has a blood volume approximately the size of a can of coke. Did you know that about 20-30% of the baby’s blood volume is still in the placenta after they’re born (Wickham, 2020)? And that’s the good stuff! We don’t want to deprive baby of that rich, oxygenated blood by clamping and cutting prematurely. Rather, wait until the cord has stopped pulsing and gone white-ish. It’s actually kind of neat to watch that last little bit of nutrients, the starting blocks of life, being pumped into baby while they rest on your chest. There’s no rush for cutting that cord. You can wait up to an hour, should you wish (Odent, 2020). If the placenta is still inside you, keep baby on your chest and enjoy the pure elation you’re feeling! If the placenta has come out, it can simply sit in a bowl beside you and baby on the bed until the Golden Hour is complete. There’s no rush to cut!
There’s also no need to worry about where baby is in relation to the placenta. It used to be standard practice that baby be held below the level of the placenta until the cord is cut, but this is outdated and proven another unnecessary hindrance (LaPoint, 2017). So get those sweet snuggles in without worry!
Here are some more reasons to wait to cut the cord! Studies show that waiting to cut the cord can reduce breathing difficulties for baby and require less need for supplemental oxygen, ventilation, and blood transfusion. Other benefits include an improvement in their cardiac (heart) function, an increase in the baby’s iron stores, neurological advantages and can lead to a baby receiving almost a billion more stem cells (Wickham, 2020).
2. IMMEDIATE SKIN TO SKIN
There are so many benefits to immediate skin to skin contact with baby after your birth. This powerful and intimate connection helps newborns adjust to being outside the womb. For baby, studies show they have greater respiratory readings, temperature regulation, glucose stability, better breastfeeding and significantly less crying (Nawal, 2020 & Phillips, 2013). Other literature indicates that conducting skin to skin practices during the Golden Hour contributes to neonatal thermoregulation with higher newborn assessment scores (Neczypor, 2017). For you, having baby skin to skin in a quiet and safe space promotes the flow of oxytocin (the love hormone), which is necessary for the release of your placenta. Encouraging your flow of oxytocin helps minimize the risk of postpartum hemorrhaging by ensuring the placenta comes out intact.
Having baby immediately placed on your bare chest means you can breathe in that sweet baby essence from the top of their head. Sometimes, that’s the only area of their body you have access to since, at this point, baby is still attached to the cord, which is still attached to the placenta inside you. As I said above, oxytocin contracts your uterus and it’s important for the placenta to come out intact to avoid postpartum hemorrhaging (Nawal, 2020). So help your uterus by taking in that sweet smell or gazing into baby’s eyes by keeping them skin to skin.
Another great benefit when baby gets placed on your bare chest is their attraction to the Montgomery’s glands (little bumps around the areola + nipple). Those glands secrete a smell that’s similar to amniotic fluid, which is why baby instinctively starts to root around that area! When baby roots around the nipple, it also triggers the release of oxytocin to help release your placenta. See how important it is to allow the post-birth process to unfold without so much unnecessary interference? Remember, birth is a natural process!
And lastly, babies who are kept skin to skin immediately after birth for at least an hour, are more likely to latch to the breast (Svensson, 2013; Crenshaw, 2014). It also helps your colostrum (the first milk that is full of nutrients that protect baby) to flow more easily. If you’re planning on breastfeeding, this can mean a profound advantage to learning this new venture! A study conducted in 2014 explores the functioning of the uterus during the 3rd and 4th stages when skin-to-skin contact and breastfeeding occurs and when it does not (Saxton 2014). It concludes, “that all women and babies should be enabled and supported to have immediate and prolonged skin-to-skin contact and breastfeeding at birth” (Saxton 2014).
3. NO HATTING
Hatting newborns became normalized in the days of twilight sleep births when the babies were taken from their drugged mothers to be “cleaned-up”, swaddled and hatted because skin to skin was not an option and baby can have difficulties regulating their body temperature. There are studies from over 40 years ago that indicate putting a Gamgee-lined hat (wool hat lined with a single layer of Gamgee) on a baby who is lying naked can help them regulate temperature (Chaput, 1979). The conclusions of this test state, “Gamgee-lined hats should be routinely used to minimise heat loss, especially in small infants exposed at birth, during surgical operations, and during investigations necessitating prolonged exposure” (Chaput, 1979). Full-term healthy babies who do skin to skin with a warm blanket covering both mother and baby were not included in this test. Because these tests were not performed skin to skin, how can we assume that hats would be more beneficial than skin to skin?
Another study done in 1979 (Coles, 1979) concluded, “It seems therefore that the stockinette hats are unlikely to be of any value in reducing heat loss immediately after birth, but that Gamgee-lined hats are effective”. So unless you’re hating baby with a wool hat, it’s not an effective practice, rather, it just interferes with the mother-child bond. That’s a lot to think about since here in Canada, we only use stockinette hats in hospitals.
But don’t humans lose most of their heat from their heads? That was debunked in 2006. This particular study indicates “whole head submersion in 17°C water did not contribute relatively more than the rest of the body to total surface heat loss” (Pretorius, 2006). This study, coupled with another in 2010, “shows that skin-to-skin care implies better thermal regulation” are strong arguments to support the conclusion that hatting is not necessary during skin to skin (Marín, 2010).
Moreover, there is sufficient evidence to conclude that oxytocin and our olfactory system are closely linked (Oettl, 2017). By smelling the essence from the top of baby’s head, it helps release necessary hormones to complete the third stage of labour successfully (BellyBelly2020). A study in 2003 discovered that the magical new baby scent creates a pleasurable response in a new mother’s brain (Lundström, 2013). Pleasure is another way to help release oxytocin. That’s why it’s called the love hormone!
A study done in 2013 states, “the scent of a newborn infant is able to elicit increased responses in the brain’s neostriatal areas within women that in previous studies have been closely linked with reward learning mechanisms” (Lundström, 2013). This is where we see bonding between infant and mother grow. Another great reason to ditch the hat and smell baby’s head!
Bonding isn’t the only benefit of sniffing that newborn smell. As mentioned above, during the third stage of labour is when the placenta is birthed. The cue to expel the placenta is triggered by a big sniff of your baby’s head. Oxytocin floods and you safely birth your placenta. When we leave the body alone to birth naturally, we really see how amazing this vessel truly is!
4. RUB VERNIX IN, NOT OFF
Some babies are born with a thick, white, cheese-like substance on their skin. It begins to appear at about 20 weeks in utero and it helps protect baby’s skin from the amniotic fluid. A study about the properties of vernix indicate that, “a total of 41 proteins, of which 25 are novel to vernix, have been detected. Effectively, 39% of identified vernix proteins are components of innate immunity and 29% have direct antimicrobial properties” (Singh, 2008). How truly amazing our bodies are to produce this powerhouse substance? So why would we wipe it off?
Other benefits of vernix are: fights germs and pathogens, protects from meconium exposure, helps regulate baby’s temperature, moisturizes and keeps skin soft and acts a lubricant while baby is passing through the birth canal, resulting in less birth trauma (Howland, 2019).
5. QUIETUDE IN BIRTHING SPACE
Part of helping to promote the flood of oxytocin after baby arrives means allowing mother to stay in “Birth Land”, a surreal place where she is solely focussed on baby and bonding. This happens during the Golden Hour! Right after baby is born, it is essential to have the room quiet and allow the shift from woman to mother to take place. This is such a sacred time and science now shows the long lasting effects that the Golden Hour has for both baby and mom’s health so keep it quiet to help honour this time (Odent 2020).
6. NEWBORN ASSESSMENT DONE ON MOM
After baby arrives, the midwife or pediatrician will do an APGAR score on your baby. You likely won’t even know they’re doing it. This score indicates if the baby is in good health after birth. It used to be standard practice to take baby and have the caregiver score them away from the mother, but the APGAR test can be conducted with baby on your chest doing skin to skin. Sometimes all you have to do is ask!
In conclusion, the female body is a powerhouse. This vessel knows how to birth. It’s innate! And for healthy term babies and uncomplicated births, it’s important to allow the post-birth process to unfold naturally without unnecessary interference. Remember, birth is a natural process!
And lastly, getting informed doesn’t have to stop after you leave your prenatal appointment. Doctors and midwives are busy and it’s their job to help you medically. Emotional and mental support cannot be expected of your doctor. That said, this reality should NOT stop you from asking the questions—sometimes all you need to do is ask! Knowledge is power, right?
Remember, this is your birth. You get to make the decisions about this journey, so get informed and ensure your questions, queries and decisions are supported by your caregiver. This is the root of Informed Choice, which I’ll save for another article!!!
References
Raylene Phillips, The Sacred Hour: Uninterrupted Skin-to-Skin Contact Immediately After Birth,
Newborn and Infant Nursing Reviews, Volume 13, Issue 2, 2013, Pages 67-72
Sara Wickham, Nadine Edwards, The Benefits of Waiting, Midwifery Today, Issue 133, Spring 2020
E C Coles, H B Valman Br Med J. 1979 September 22; 2(6192): 734–735
BeelyBelly, Hats On Newborn Babies: Reasons To Ditch The Hatby BellyBelly, May 17, 2022
Genevieve Howland, Vernix: Don’t Wash It Off, Rub It In, May 24, 2019
**This is not medical advice. These topics are intended to help you have an informed birthing experience. Talk to your caregivers, do your research, hire a doula and make each choice about your birth experience with confidence and empowerment.